The most usual surgical conditions of anus and perineum are pilonidal disease, haemorrhoids, anal fissure, perianal abscess and perianal fistula. They are very frequent conditions that affect a large portion of the population.
These conditions although they are not life threatening, they cause very intense and bothering symptoms, while their anatomic location makes them very difficult to be tolerated, especially by young and active patients.
More than one of these conditions often exist in the same patient. They can be treated simultaneously and by applying the principals of minimally invasive surgery by specialised surgical teams, offering permanent solution in complex problems.
Pilonidal Disease
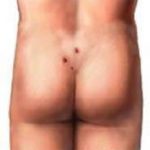
With this term we describe a chronic inflammation of the skin between the haunches, which is caused by hair infiltration into the skin, resulting in a chronic abscess of the area.
It is more often affecting young and hairy patients. Frequency elevates in obese patients.
Usual symptoms
It is initially manifested as a painful bulge which is later transformed in a chronic abscess with outflow of bad smelling, bloody and pus content.
The disease has outbursts and recessions and every time the size of the lesion is getting bigger, affecting more and more the surrounding healthy tissue.
Treatment
Treatment is exclusively surgical. The surgeon performs complete excision of the abscess and the surrounding fistulas. The procedure is made under local anaesthesia and it usually demands a few hour hospitalisation.
The procedure is performed either with the conventional way or by applying laser and radio waves. During the post-surgical course, frequent assessments of the wound are made, in order to keep the wound clean and heal in a 2-3 week course.
Successful results (without recurrence), post-surgical pain and healing time depend directly on the techniques applied by the surgeon, manifesting big differences among the various “surgical schools”.
Today we can safely suggest that unlike the recent past, pilonidal cyst can and must be treated painless and with short-term healing period.
Modern tools and techniques that have been perfected through time give us the potential to offer the patient permanent treatment combined with less post-surgical pain and drastic reduction of the recovery course.
Haemorrhoids

Haemorrhoids locate at the anus, being a natural anatomic element. In fact they are a network of veins carrying blood all over the anal canal. This complex of vessels is called “haemorrhoid plexus” and during defecation it is swollen and acts as protective pillow in the sphincter ring, which is responsible for the continence during the day and also allows stool to go out during defecation. They cause symptoms when they are swollen and the tissues that keep them in place relax, resulting to their protrusion under the anal ring.
Almost every individual during its lifetime will percept the existence of haemorrhoids, with the one third of them needing treatment to be relieved of the symptoms that they cause. Haemorrhoids are distinguished in internal and external, according to their location and if they protrude from inside the anal ring. Also, concerning their size and the protrusion from the sphincter they are distinguished in four degrees, from 1st degree which is normal, to 4th degree which represents haemorrhoids permanently protruding through the anal ring and not able to put in place even with external pressure.
Predisposing factors for the appearance of haemorrhoids are:
- Low fibre diet
- Lack of physical exercise
- Elevated intra-abdominal pressure (e.g. obesity, heavy craftwork)
- Pregnancy
- Chronic constipation or transient diarrhoea.
- Drugs causing constipation or diarrhoea.
- Family history.
Usual symptoms include:
- Anal pain
- Bleeding
- Sphincter relaxation with mild incontinence and mucous secretion
- Local irritation and itching
- Swelling and protrusion
Treatment
Conservative management: Conservative management aims at the relief from symptoms (itching, burning, bleeding, mucous, pain) and not the treatment of haemorrhoids. It includes good hygiene of the anal and perianal region and avoiding constipation by consuming high fibre diet. In case of inflammation, local anti-inflammatory ointments and venotonic drugs are used to facilitate the blood outflow from the area.
Surgical treatment: It is indicated in cases where the symptoms reoccur and it is the only way to make haemorrhoids disappear, along with the symptoms of course.
The most usual techniques are:
Haemorrhoidectomy using Laser, microwaves or ultrasound..
It represents the evolution of the classical techniques (Milligan-Morgan, Ferguson) and is a radical but also painful procedure, during which every swollen haemorrhoid is excised at the level of the sphincter followed by the sewing of the anal skin.
Longo Haemorrhoidectomy.
In this technique haemorrhoids are not excised at the level of the sphincter, but with the use of a special stappling device, their vascularisation is disrupted at a depth of 7-8cm and they are simultaneously retracted upwards. It is accompanied by mild post-operative pain, since they don’t traumatise the sphincter area.
Devascularisation haemorrhoidectomy THD and HAL..
With these techniques (Transanal Haemorrhoidal Dearterialization) the main haemorrhoidal arteries are ligated under ultrasound guidance. This technique is bloodless, minimally invasive, uncomplicated, and quick and allows the patient to return in his daily routine in one day. Transanal haemorrhoid ligation and haemorrhoidopexy is a method which relieves the patient without incisions, pain and complications that follow the classical methods, while it simultaneously resolves the prolapse of the haemorrhoidal nodules.
Minimal wound of the area, bloodless procedure and lack of post-operative pain make this procedure selection of choice for the treatment of haemorrhoids.
Anal fissure
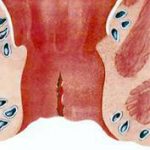
It is a linear, painful lesion of the anal canal extending to the level of the internal sphincter of the anus. It exists in both men and women. It is manifested with extreme pain just after defecation (like tear or burn), which can last for several hours and sometimes is accompanied by bleeding.
Main pathogenic factor is considered the trauma of the anal skin during defecation (mostly in cases of chronic constipation), combined with anal sphincter hypertension. Rarely, it is caused by inadequate healing after surgical procedures in the area and local trauma. Conservative treatment with laxatives and ointments usually fails and surgical treatment is commonly necessary.
Surgical treatment is performed with use of Laser or radiofrequency by a specialised surgeon, methods that allow the bloodless treatment of fissure. Apart from excision of the fissure, partial lateral internal sphincterotomy is also usually performed, eliminating the chronic spasm of the sphincter and facilitating the rapid healing and also contributes to the avoidance of recurrence. The procedure is fast and the patient returns to daily activities after few hours.
Perianal abscess
Perianal abscess is formed when a small rupture of the lumen of the bowel occurs, near the anus. This results to the formation of a localised septic collection which is evolving to an abscess. It is manifested with intense pain, fever, redness and pus collection in the area around the anus, as a result of acute and intense septic inflammation.
If not treated, it is possible to cause fistula or gangrene of the perianal area. The treatment is exclusively surgical and involves opening and drainage of the abscess cavity.
Perianal fistula
Perianal fistula is the tunnel between the bowel (internal orifice) and the skin (external orifice). It is usually manifested with pus outflow from the external orifice. It is almost always a result of insufficient treatment of perianal abscess. As it becomes chronic, it causes itching and skin lesions due to the pus outflow.
The treatment of fistula is always surgical. It is consisted of the full recognition of its course and the excision of both the internal and external orifice, as well as the intermediate tunnel. Special care must be taken to protect the sphincter and avoid injuries to it, in order to maintain its full function.
 With this term we describe a chronic inflammation of the skin between the haunches, which is caused by hair infiltration into the skin, resulting in a chronic abscess of the area.
It is more often affecting young and hairy patients. Frequency elevates in obese patients.
Usual symptoms
It is initially manifested as a painful bulge which is later transformed in a chronic abscess with outflow of bad smelling, bloody and pus content.
The disease has outbursts and recessions and every time the size of the lesion is getting bigger, affecting more and more the surrounding healthy tissue.
With this term we describe a chronic inflammation of the skin between the haunches, which is caused by hair infiltration into the skin, resulting in a chronic abscess of the area.
It is more often affecting young and hairy patients. Frequency elevates in obese patients.
Usual symptoms
It is initially manifested as a painful bulge which is later transformed in a chronic abscess with outflow of bad smelling, bloody and pus content.
The disease has outbursts and recessions and every time the size of the lesion is getting bigger, affecting more and more the surrounding healthy tissue.
 Haemorrhoids locate at the anus, being a natural anatomic element. In fact they are a network of veins carrying blood all over the anal canal. This complex of vessels is called “haemorrhoid plexus” and during defecation it is swollen and acts as protective pillow in the sphincter ring, which is responsible for the continence during the day and also allows stool to go out during defecation. They cause symptoms when they are swollen and the tissues that keep them in place relax, resulting to their protrusion under the anal ring.
Almost every individual during its lifetime will percept the existence of haemorrhoids, with the one third of them needing treatment to be relieved of the symptoms that they cause. Haemorrhoids are distinguished in internal and external, according to their location and if they protrude from inside the anal ring. Also, concerning their size and the protrusion from the sphincter they are distinguished in four degrees, from 1st degree which is normal, to 4th degree which represents haemorrhoids permanently protruding through the anal ring and not able to put in place even with external pressure.
Predisposing factors for the appearance of haemorrhoids are:
Haemorrhoids locate at the anus, being a natural anatomic element. In fact they are a network of veins carrying blood all over the anal canal. This complex of vessels is called “haemorrhoid plexus” and during defecation it is swollen and acts as protective pillow in the sphincter ring, which is responsible for the continence during the day and also allows stool to go out during defecation. They cause symptoms when they are swollen and the tissues that keep them in place relax, resulting to their protrusion under the anal ring.
Almost every individual during its lifetime will percept the existence of haemorrhoids, with the one third of them needing treatment to be relieved of the symptoms that they cause. Haemorrhoids are distinguished in internal and external, according to their location and if they protrude from inside the anal ring. Also, concerning their size and the protrusion from the sphincter they are distinguished in four degrees, from 1st degree which is normal, to 4th degree which represents haemorrhoids permanently protruding through the anal ring and not able to put in place even with external pressure.
Predisposing factors for the appearance of haemorrhoids are:
 It is a linear, painful lesion of the anal canal extending to the level of the internal sphincter of the anus. It exists in both men and women. It is manifested with extreme pain just after defecation (like tear or burn), which can last for several hours and sometimes is accompanied by bleeding.
Main pathogenic factor is considered the trauma of the anal skin during defecation (mostly in cases of chronic constipation), combined with anal sphincter hypertension. Rarely, it is caused by inadequate healing after surgical procedures in the area and local trauma. Conservative treatment with laxatives and ointments usually fails and surgical treatment is commonly necessary.
Surgical treatment is performed with use of Laser or radiofrequency by a specialised surgeon, methods that allow the bloodless treatment of fissure. Apart from excision of the fissure, partial lateral internal sphincterotomy is also usually performed, eliminating the chronic spasm of the sphincter and facilitating the rapid healing and also contributes to the avoidance of recurrence. The procedure is fast and the patient returns to daily activities after few hours.
It is a linear, painful lesion of the anal canal extending to the level of the internal sphincter of the anus. It exists in both men and women. It is manifested with extreme pain just after defecation (like tear or burn), which can last for several hours and sometimes is accompanied by bleeding.
Main pathogenic factor is considered the trauma of the anal skin during defecation (mostly in cases of chronic constipation), combined with anal sphincter hypertension. Rarely, it is caused by inadequate healing after surgical procedures in the area and local trauma. Conservative treatment with laxatives and ointments usually fails and surgical treatment is commonly necessary.
Surgical treatment is performed with use of Laser or radiofrequency by a specialised surgeon, methods that allow the bloodless treatment of fissure. Apart from excision of the fissure, partial lateral internal sphincterotomy is also usually performed, eliminating the chronic spasm of the sphincter and facilitating the rapid healing and also contributes to the avoidance of recurrence. The procedure is fast and the patient returns to daily activities after few hours.


